ORIGINAL RESEARCH
Etiological structure of enterovirus infection in children in the Moscow region
1 Center for Strategic Planning and Management of Medical and Biological Health Risks of the Federal Medical Biological Agency, Moscow, Russia
2 Speransky Children's City Clinical Hospital No. 9, Moscow, Russia
The diversity and succession of epidemiologically significant enteroviruses (EV) lead to constant changes in the clinical presentation and morbidity levels. The aim of the study is to investigate cases of EV infection in hospitalized children during the resurgence of the epidemic process following the COVID-19 pandemic. We collected clinical samples from 156 patients with EV infection across a range of ages. Virus genotyping was performed using the Sanger sequencing of the 5’UTR-VP2 and VP1 genome fragments. Sixteen types of enteroviruses were identified, with one additional case identified only to the species level (EV-C). The dominant EV type was Coxsackie CV-A6, with a share of 80.6% (95% CI: 66.7–95.5) in 2021 and 36.1% (95% CI: 27.5–44.6) in 2022. Most commonly, CV-A6 caused skin lesions (exanthema or HFMD) and respiratory manifestations. In 2022, the proportion of CV-A10 cases increased considerably to 27.0% (95% CI: 19.2–34.9) compared with 6.4% (95% CI: 0–15.1) in 2021. The most common clinical manifestation of CV-A10 was herpangina. The most severe EV infection cases were associated with ECHO 6 — four out of 11 patients were diagnosed with meningitis, while the remaining patients exhibited neurological symptoms (meningism, intense headache, vomiting) accompanied by fever. We observed a large number of EV cases accompanied by the presence of other infectious agents in biological samples, which may result from immune suppression during EV infection development. The most common of these agents was human herpesvirus 6 (HHV-6). The nucleotide sequences of the characterized enteroviruses have been deposited in the NCBI database to enable subsequent epidemiological analysis of enterovirus circulation in the Russian Federation.
Keywords: Sanger sequencing, enterovirus infection, epidemiologically significant enteroviruses, hand, foot and mouth disease (HFMD), herpangina, Coxsackie viruses, Echoviruses, co-infection
Author contribution: Polyakova VA, Luparev AR, Matsvay AD, Gnusareva NI, Gordukova MA, Galeeva EV, Tolokonceva AA — conducting the research; Davydova EE, Polyakova VA, Luparev AR — literature analysis; Davydova EE, Luparev AR — data interpretation; Gordukova MA, Galeeva EV — collection of biological samples; Polyakova VA — article authoring; Davydova EE — manuscript editing; Polyakova VA — preparation of illustrations; Shipulin GA — supervision and procurement of funding.
Compliance with ethical standards: the study was approved by the Ethics Committee of the Children's City Clinical Hospital No. 9 named after G.N. Speransky (Minutes No. 44 of April 19, 2022), conducted in accordance with the principles of the Declaration of Helsinki. All participants submitted signed informed consent forms prior to participation in the study.
Correspondence should be addressed: Ekaterina E. Davydova
Pogodinskaya, 10, Moscow, 119121, Russia, еur.abmfpsc@avodyvad
Enteroviruses are a diverse group of small non-enveloped viruses with an non-segmented (+)-RNA genome, including pathogenic and opportunistic human viruses of the species Enterovirus alphacoxsackie (EV-A), Enterovirus betacoxsackie (EV-B), Enterovirus coxsackiepol (EV-C), Enterovirus deconjuncti (EV-D). Polioviruses belonging to the Enterovirus coxsackiepol species, capable of causing severe forms of neuropathogenesis, are on the verge of elimination. However, non-poliomyelitic enteroviruses of various types, including Coxsackie viruses, echoviruses and numbered enteroviruses, are widespread, and they cause various clinical forms of enterovirus infection, including hand, foot and mouth disease (HFMD), various types of exanthema, herpangina (enterovirus vesicular pharyngitis), diseases of the upper and lower respiratory tract, hemorrhagic conjunctivitis, infections of the gastrointestinal tract, epidemic myalgia, myopericarditis, neuroinfections (encephalitis, meningitis, acute flaccid myelitis) and other diseases.
A certain correlation has been established between the species of enteroviruses and their characteristic clinical manifestations: EV-A enteroviruses predominantly cause HFMD and herpangina; EV-B enteroviruses (Coxsackie B, ЕСНО) are the dominant pathogens of enterovirus meningitis; EV-D enteroviruses (D68) mainly affect the upper and lower respiratory tract. However, even for a single type of enterovirus, the clinical picture can vary significantly depending on the state of immunity and other individual characteristics of the patient. Approximately 85 % of EV infection cases are asymptomatic, about 12–14 % are diagnosed as mild forms, and only 1–3 % exhibit a severe course [1, 2]. Clinical manifestations are also associated with certain age groups: in adult patients, the disease often occurs as a mild respiratory or intestinal infection, younger patients develop HFMD, herpangina, and exanthema, and children aged 3-14 years are predisposed to severe neurological forms, such as enterovirus meningitis [2].
Monitoring of EV infections reveals that distinct circulation patterns exist for individual enterovirus types; for example, ECHO 9, ECHO 30, and EV-D68 tend to cause outbreaks, whereas CV-B4 and several other types exhibit relatively stable circulation [2, 3].
The regular replacement of epidemiologically important enterovirus may stem from different factors, but it always affects the incidence rate and the nature of the clinical picture. Monitoring the activity and prevalence of different EV types allows predicting the emergence of outbreaks or an increase in severe disease cases. [1, 4].
In 2020, the COVID-19-related anti-epidemic measures slowed the circulation of enteroviruses. Consequently, in the subsequent years, the proportion of the population without immunity to enterovirus infection increased, which contributed to a more active spread of EV infection. Thus, according to official statistics in the Russian Federation, in 2024, there were 21491 EV cases recorded, which is 14.69 per 100 thousand population. This is 1.5 times more than the long-term baseline incidence rate [5].
Before the pandemic, EV-B enteroviruses, including ECHO 30, posed a significant threat in the Russian Federation, being a major cause of meningitis. However, following the decline in enterovirus circulation in 2020, the proportion of EV-B decreased significantly. At the same time the incidence of infections associated with EV-A, primarily A6 and A10, has increased [2, 6]. According to the data of molecular genetic monitoring in the Russian Federation, in some years, the share of CV-A6 reached 40% [2, 7]. In this regard, the clinical presentation of EV infections has also changed, cases of herpangina and exanthema becoming more frequent, especially among children in their early years [6]. For example, in the Irkutsk region in 2023, the main clinical form of EV infection was herpangina (39.9%) and HFMD (28.9%) [8].
The aim of the study is to investigate cases of EV infection in children admitted to hospitals in the Moscow region during the period of epidemic process recovery (2021–2023), in order to assess the circulation of various enterovirus types taking into account the associated clinical manifestations.
METHODS
Samples
Clinical samples were collected from 156 patients of various ages at the Children's City Clinical Hospital No. 9 named after G. N. Speransky (Moscow, Russia). The participants had to have a diagnosed enterovirus infection to be included in the study. The children were aged 0–17 years; 78% of them were under six years of age. Most of the samples (n = 122) were collected in 2022, with additional 31 and 3 samples taken in 2021 and 2023.
Oropharyngeal and nasopharyngeal swab samples (n = 137) were collected from patients with symptoms of EV or respiratory infection, feces (n = 18) were taken from patients with acute intestinal infection. A cerebrospinal fluid sample was taken from one patient diagnosed with meningitis (n = 1). Only one type of clinical specimen was analyzed per patient. Clinical specimens were stored at –70 °C until the start of the analysis.
Study locations
PCR testing of samples for the presence of enterovirus RNA and other infectious agents was performed in the Laboratory Diagnostic Department of Children's City Clinical Hospital No. 9 named after G. N. Speransky. Enterovirus genotyping was performed in the Center for Postgenomic Technologies of the Center for Strategic Planning and Management of Medical and Biological Health Risks (FMBA of Russia).
Sample preparation
Swab and cerebrospinal fluid samples did not require any preparation before RNA extraction. To prepare the fecal extract, approximately 0.1 g (0.1 ml) of feces was resuspended in 0.8 ml of phosphate buffer (VWR International, LLC, USA). The homogeneous suspension was centrifuged at 10000 g on a MiniSpin centrifuge (Eppendorf, Germany) for 5 minutes, 300–400 µl of supernatant was collected above the surface of the precipitate, and stored at –70 °C for further use.
Confirmation of the presence of enterovirus and other infectious agents in clinical samples
To confirm the presence of enteroviruses and other infectious agents in clinical samples, we used PCR kits AmpliTest® Neuroviruses (Center for Strategic Planning and Management of Medical and Biological Health Risks, FMBA of Russia, Russia), AmpliSens® EBV/CMV/HHV6A/B-screen-FL, AmpliSens® HSV I, II-FL, AmpliSens® OKI-screen-FL, AmpliSens® ARVI-screen-FL, AmpliSens® MRSA-screen-titer-FL, AmpliSens® Streptococcus pyogenesscreen/monitor-FL (Central Research Institute of Epidemiology of Rospotrebnadzor, Russia).
RNA extraction
For nucleic acid extraction from clinical samples, the in vitro diagnostic reagent kit AmpliTest® Magno-Sorb-Combo (Center for Strategic Planning and Management of Medical and Biological Health Risks FMBA of Russia, Russia) was used. The set extracts nucleic acids using magnetized silica particles. RNA isolation was performed using the Auto-Pure 96 device (Hangzhou Allsheng Instruments Co., Ltd., China). For extraction, 10 µl IC-R was added to all the samples.
Obtaining cDNA
Reverse transcription of RNA was performed using the AmpliTest® Reverta kit (CSP of FMBA of Russia, Russia).
Amplification of 5'UTR-VP2 and VP1 regions of the enterovirus genome
The VP1 region was amplified using universal primers recommended for genotyping human enteroviruses EV-A, EV-B, EV-C, and EV-D. The process involved two-round thermal cycling: the first round with a pair of primers SO222 5’-CICCIGGIGGIAYRWACAT-3’ and SO224 5’-GCIATGYTIGGIACICAYRT-3’, and the second round with AN88 5’-TACTGGACCACCTGGNGGNAYRWAC AT-3’ and AN89 5’-CCAGCACTGACAGCAGGARAYNGG-3’ [9]. To amplify the 5'UTR-VP2 region of the enterovirus genome, we used oligonucleotide primers of our own design — EV_S_for 5’-GTGTAGMTYRGGYYGATGAG-3’ and EV_S_rev 5’-RTCHGGRAAYTTCCAVYACCA-3’.
Electrophoretic analysis of PCR products and their purification
Electrophoresis of PCR products was carried out in 2% agarose gel. For purification of PCR products, we used KAPA Pure Beads (KAPA Biosystems, Wilmington, MA, USA). Nucleic acid concentrations were measured using a NanoDrop 2000C spectrophotometer (Thermo Scientific, Waltham, MA, USA).
Sequencing of sections of the enterovirus genome
The Sanger PCR reaction was carried out using the BigDye™ Terminator v3.1 Cycle Sequencing Kit (Thermo Fisher Scientific) in accordance with the manufacturer’s protocol on a SimpliAmp Thermal Cycler (Thermo Fisher Scientific). For sequencing of VP1 and 5'UTR-VP2 PCR products, we used internal primers AN232 5’ CCAGCACTGACAGCA 3’ [9] and EV_S_in 5’ CATGGTGYGAAGYCTATTGAGC 3’ respectively. The Sanger sequencing was performed on an Applied Biosystems 3500 Genetic Analyzer (Thermo Fisher Scientific).
Enterovirus RNA was found in 156 clinical samples. Genotyping in two genome regions was performed for 96 samples; the results of VP1 and 5'UTR-VP2 typing were the same for all of them. For 40 samples, genotyping was performed only in the 5'UTR-VP2 region, and for 20 samples in the VP1 region of the genome.
The nucleotide sequences of fragment VP1 (PX468781– PX468895) and region 5'UTR-VP2 (PX491339–PX491474) were uploaded to the NCBI GenBank database.
Identification of enterovirus types
We used the resources of Enterovirus Genotyping Tool Version 0.1, National Institute for Public Health and the Environment, Bilthoven, The Netherlands) [10] and NCBI BLAST [11].
Statistical data processing
We used the Medcals resource [12] and the standard functions of Microsoft Excel (Microsoft Corporation). To compare the frequency of symptoms between the groups, the two-tailed Fisher’s exact test was performed. Differences were considered statistically significant at p < 0.05. For samples with a small number of observations (n < 10), no statistical comparison was performed.
RESULTS
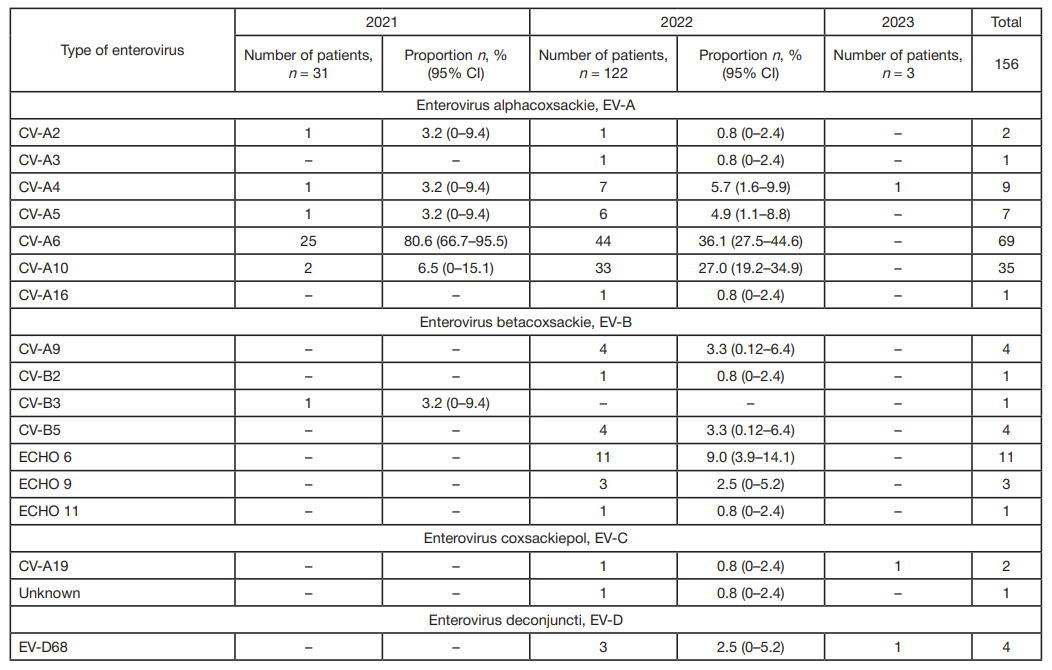
Genotyping of enteroviruses in biological samples from children revealed 16 different types, for one sample only the EV-C enterovirus species could be established. The majority of the studied enteroviruses were of the EV-A CV-A6 type: among the samples from 2021, their share was 80.6%, from 2022 — 36.1%. CV-A10 was the second most common enterovirus detected in EV patients, accounting for 6.5% of the 2021 sample batch and 27.0% of the 2022 batch. Other EV-A enteroviruses were found much less frequently. The CV-A16 virus was detected in only one patient (2022 sample batch).
EV-B viruses of types CV-A9, CV-B2, CV-B3, CV-B5, ECHO 6, ECHO 9, ECHO 11 were identified in 16.0% of patients (in 2021-2022). ECHO 6 dominated among them, with a 9.0% share in the 2022 sample batch.
In addition, we identified three samples of enterovirus of the EV-C species (two cases of CV-A19 and one case of EV-C of unidentified type) and four cases of enterovirus EV-D68 of the EV-D type. The results of enterovirus genotyping are shown in tab. 1.
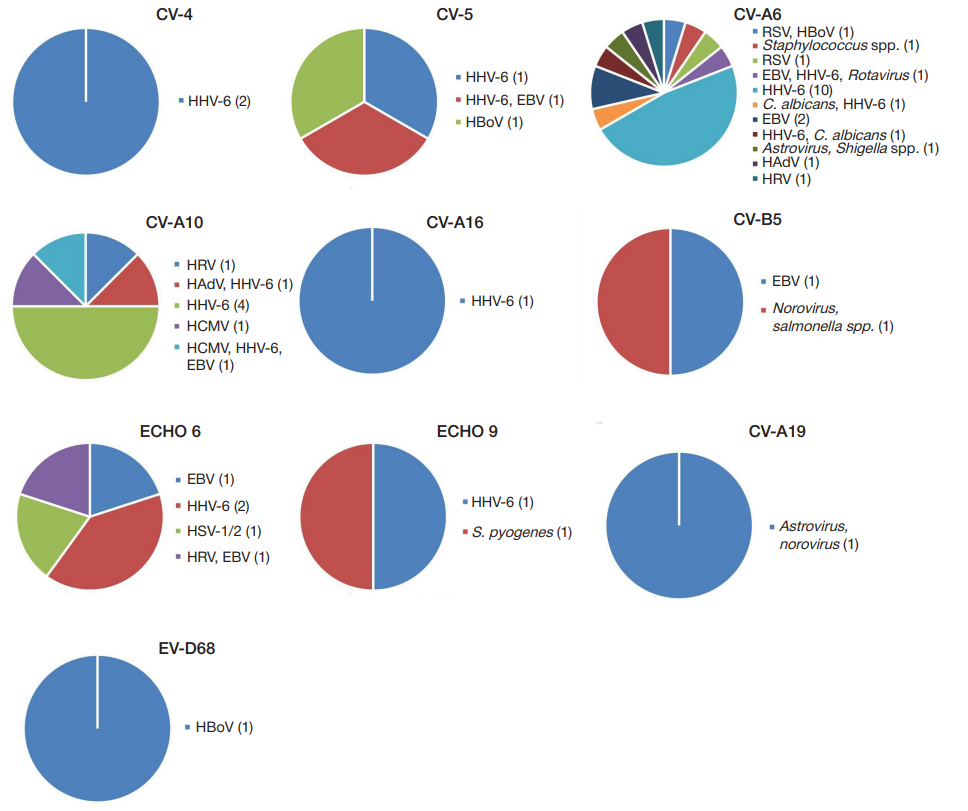
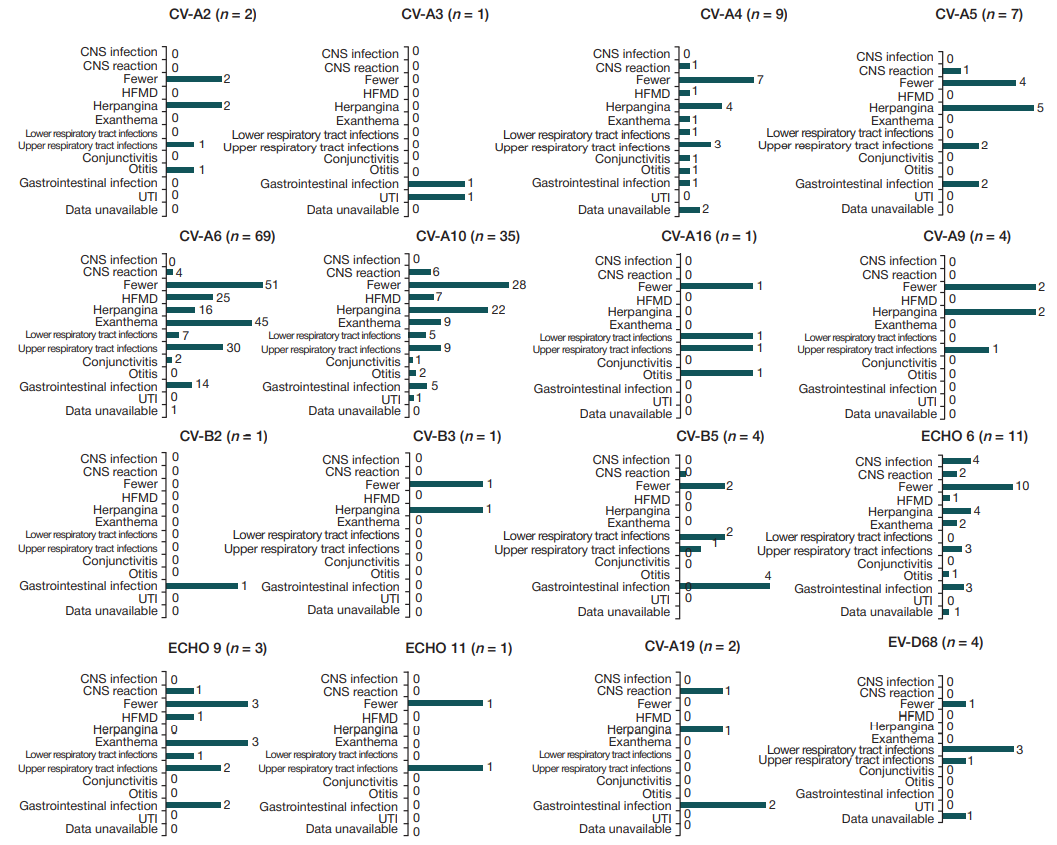
We analyzed the relationship of symptoms in patients infected with enteroviruses of various types. Those of the EV-A species (CV-A2, CV-A3, CV-A4, CV-A5, CV-A6, CVA10, CV-A16) caused similar symptoms: HFMD, exanthema, diseases of the upper and lower respiratory tract, herpangina, gastrointestinal infections, acute hemorrhagic conjunctivitis. Enteroviruses of the EV-B type (CV-A9, CV-B2, CV-B3, CV-B5, ECHO 6, ECHO 9, ECHO 11) mainly manifested as neurological disorders (meningism, intense headache, vomiting) against a background of fever, respiratory and/or intestinal symptoms. Four of the 11 patients with ECHO6 infection were diagnosed with meningitis (fig. 1).
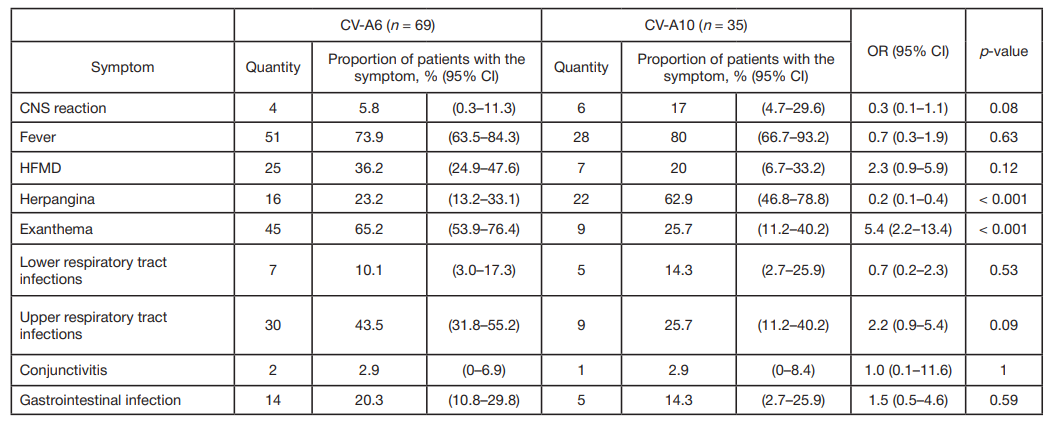
Enteroviruses of types СV-A6 (n = 69) and CV-A10 (n = 35) were represented sufficiently to allow a comparison of the frequency of various clinical manifestations (tab. 2). It was reliably shown that in this study, exanthema developed more often in patients with CV-A6 infection than in CV-A10 cases (65.2% vs 25.7%), and herpangina, on the contrary, was more often observed when the disease was brought by a CV-A10 infection (62.9% vs 23.2%).
We have also investigated the frequency of detection of other infectious agents in patients, including those causing a clinical picture similar to an EV infection (exanthema, respiratory, intestinal, or neuroinfections). The specific RNA and DNA pathogens tested for were as follows: herpes simplex viruses type 1 and 2 (HSV-1/2), human herpesvirus 6 (HHV-6), Epstein– Barr virus (EBV), cytomegalovirus (HCMV), rhinoviruses (HRV), respiratory syncytial virus (RSV), human metapneumovirus (HMPV), human parainfluenza viruses types 1–4 (HPIV-1 to HPIV-4), human bocavirus (HBoV), adenoviruses species B, C, E, and F (HAdV-B, -C, -E, -F), human coronaviruses OC43, 229E, NL63, and HKU1 (HCoVs), rotavirus A, norovirus genogroup II, astroviruses, Shigella spp./enteroinvasive Escherichia coli (EIEC), Salmonella spp., Campylobacter spp., Streptococcus pyogenes, Staphylococcus spp., and Candida albicans.
The total number of EV infection cases concomitant with other infectious agents in various combinations was 29.5%, but in most cases, those agents did not significantly affect disease severity. Herpes virus type 6 (HHV-6) was detected most often (in up to 17% of all studied cases of EV infection). In 7% of cases, we observed infections involving multiple pathogens — either mixed viral infections (e.g., CV-A10, HHV-6, EBV, HCMV) or bacterial–viral co-infections (e.g., CV-A6, Astrovirus, Shigella spp.) (fig. 2).
DISCUSSION
Genotyping of enteroviruses in biological samples collected from children in the Moscow region in 2021–2022 showed that the dominant type was CV-A6. This type has been widely distributed across European countries since 2008 and subsequently spread to Asia and North America. There are atypical forms of CV-A6 that cause unusual skin manifestations: exanthema, rash, eczema, blisters, onychomadesis [13, 14]. In 2017, the prevalence of CV-A6 in some countries reached 71.1% [15], with large-scale outbreaks reported in Brazil, Vietnam, France, and China [16–20]. The dominant position of the CV-A6 in Russia is confirmed by the data of the Reference Center: the prevalence of this type among patients with EV infection was 13% in 2018, 29% in 2019, 40% in 2021, 19% in 2022, 34% in 2023, 17% in 2024 [2]. Compared to the classic Coxsackie virus CV-A16, which was previously a common cause of HFMD [2, 21], CV-A6 infection is characterized by a longer duration, atypical skin manifestations, and neurological symptoms [15, 18].
In this study, CV-A6 predominantly caused exanthema and diseases of the upper and lower respiratory tract, less often — HFMD, herpangina, gastrointestinal infections, and acute hemorrhagic conjunctivitis. In four cases (patients under 3 years old, accounting for about 6% of the CV-A6 sample), the infection was severe and accompanied by seizures and loss of consciousness in the context of febrile fever. A concomitant agent, HHV-6, was detected only in one case of these four, therefore, the complicated course is probably not associated with coinfection.
It is shown that compared to 2021, in 2022, the proportion of CV-A6 decreased from 80.6% to 36.1%, while the share of CV-A10 cases increased from 6.5% to 27.0%. This is consistent with the reports of the growing numbers of CV-A10 infection cases in the regions of the Russian Federation and other countries [2, 22, 23]. The symptoms of CV-A10 infection were generally similar to those of CV-A6 infection, except that herpangina was more frequent and various exanthemas were less common. Six patients aged 0-6 years (17% of patients with CV-A10) had seizures and/or loss of consciousness with febrile fever in the background, and only two of them had associated infectious agents (HHV-6, HAdV). In this study, we did not observe any cases of meningitis associated with CV-A10, although such cases have been reported previously. Moreover, according to published data, CV-A10 infection tends to be more severe than those caused by CV-A6 or CV-A16 [22].
Separately, it should be noted that two patients with CVA10 and CV-A3 had a rather rare complication — urinary tract infections. The cytopathogenic effect of enteroviruses on renal tissue cells was described earlier, which indicates the possibility of involvement of organs of the urinary system in the pathological process [24].
Among EV-B enteroviruses, ECHO 6 was the most common type. It was detected exclusively in the 2022 sample batch, correlating with the epidemic rise of this type observed across the Russian Federation that year [2]. Symptoms of neuroinfection were noted, some patients had meningitis, the rest had neurological symptoms (meningism, intense headache, vomiting) against the background of fever, respiratory and/or intestinal disorders. One of the cases of ECHO 6 infection manifested in a child as enterovirus vesicular pharyngitis, however, the mother of this child had it as enterovirus meningitis. This example does not agree with the typical clinical model of EV infection, in which adults carry the infection in a milder or asymptomatic form, because in the described case the parent experienced a more severe course of the disease.
In other cases of EV-B infections, the symptoms involved intestinal (gastroenteritis, enterocolitis) and respiratory (rhinitis, bronchitis) disorders without affecting the central nervous system. In some cases, we also observed herpangina (CV-B3, ECHO 6) and HFMD (ECHO 6, ECHO 9). ECHO 11, which is associated with neonatal sepsis in infants, was detected only in a three-year-old patient with symptoms of respiratory infection. The ECHO 30 virus, which has been the predominant causative agent of enteroviral meningitis in the Russian Federation for many years, was not detected in this study. This finding is consistent with the enterovirus monitoring data from the Reference Center: since the onset of the COVID-19 pandemic, ECHO 30 has been rarely detected in the Russian Federation during 2021–2022. However, ECHO 30 showed an upward trend later; in 2024, it accounted for 8% of all EV infection cases [2].
Two cases of EV-C CV-A19 virus infection have also been identified. According to the literature, CV-A19 is a fairly rare infection agent; it can cause various respiratory and intestinal disorders, herpangina, as well as meningitis and acute flaccid myelitis [25–26]. In the first case, the patient developed a herpangina with infectious enterocolitis. In the second case, against the background of norovirus and astrovirus coinfection, the child had acute infectious gastroenteritis, toxicosis, exicosis and acidosis, along with speech disorder and logoneurosis. Electroencephalography has also detected epileptiform activity. The effects affecting the central nervous system are probably associated with severe intestinal coinfection.
Epidemiologically significant enteroviruses include EV-D68, which was also identified in this study. This type commonly brings respiratory symptoms, but since 2014, it has been associated with acute flaccid myelitis, the symptoms of which include damage to the lower motor neurons in the gray matter of the spinal cord, impaired reflexes, respiratory failure, and sudden muscle weakness [27]. Outbreaks of EV-D68 infection, accompanied by acute flaccid paralysis, myelitis, myocarditis, pericarditis, neonatal sepsis, and pneumonia, have been recorded in the United States and Europe. In the Russian Federation, isolated cases of EV-D68 have been registered since 2018. The cases of EV-D68 infection identified in this study in children aged 5–12 years were associated with respiratory tract diseases, including rhinopharyngitis, obstructive bronchitis, and pneumonia.
Our data show a high proportion of cases of EV infection accompanied by other infectious agents (up to 30% of all cases), which confirms previously published data on cases of coinfections in various forms of EV infection. The literature describes cases of coinfections such as EV/HSV-1 in neonatal meningitis; CV-A6/EV-D68/HPeV/HHV-6/parvovirus in acute encephalopathy; EV/Pasteurella multocida in meningitis and sepsis; EV/HSV-1, CV-A6/HHV-7, and CV-A6 / CMV in hand, foot, and mouth disease (HFMD) syndrome; and EV / Escherichia coli in urinary tract infections [33].
According to our data, in most cases, coinfection with EV was associated with pathogens that can remain latent in the body and become active under conditions of weakened immunity — such as herpes simplex virus types 1 and 2, cytomegalovirus, Epstein–Barr virus, and human herpesvirus 6 — accounting for up to 74% of all cases in which additional infectious agents were detected.
CONCLUSIONS
It was determined that among the enteroviruses detected in children in the Moscow region in 2021–2022, CV-A6 was dominant, primarily causing skin lesions in patients. In 2022, there was an increase in the number of CV-A10 cases, for which there was a large proportion of cases with a severe course of the disease compared to CV-A6. Among EV-B viruses, the largest proportion belonged to ECHO 6; several patients were diagnosed with meningitis. A large number of EV infectious cases showed the presence of other viral and bacterial pathogens in patients' biomaterials, which may be due to immune suppression during the course of EV infectious. The nucleotide sequences of all characterized enteroviruses are publicly available in the NCBI database, which makes it possible to use them for future epidemiological analyses of enterovirus circulation in the Russian Federation.
- Alimov AV, Feldblyum IV, Akimkin VG, Zaharova Yu.A, Sergeev AG, Piterskij MV. Epidemiologicheskij nadzor i kontrol' enterovirusnoj (nepolio) infekcii: aktual'nye problemy i puti resheniya. Ekaterinburg: YUnika, 2021; 181 s, ISBN 978-5-6045184-4-1. Russian.
- Informacionnye byulleteni FBUN «Nizhegorodskij nauchno-issledovatel'skij institut epidemiologii i mikrobiologii im. akademika I. N. Blohinoj». Zabolevaemost' i etiologicheskaya struktura enterovirusnoj (nepolio) infekcii. 2021–2025. Russian.
- Khetsuriani N, Lamonte-Fowlkes A, Oberst S, Pallansch MA. Centers for Disease Control and Prevention. Enterovirus surveillance — United States, 1970–2005. MMWR Surveill Summ. 2006; 55 (8): 1–20. Available from: https://www.cdc.gov/mmwr/preview/mmwrhtml/ss5508a1.htm.
- Midgley CM, Watson JT, Nix WA, Curns AT, Rogers SL, Brown BA, et al. Severe respiratory illness associated with a nationwide outbreak of enterovirus D68 in the USA (2014): a descriptive epidemiological investigation. Lancet Respir Med. 2015; 3 (11): 879–87. DOI: 10.1016/S2213-2600(15)00335-5.
- O sostoyanii sanitarno-epidemiologicheskogo blagopoluchiya naseleniya v Rossijskoj Federacii v 2024 godu: Gosudarstvennyj doklad. M.: Federal'naya sluzhba po nadzoru v sfere zashchity prav potrebitelej i blagopoluchiya cheloveka, 2025; 2025. Russian.
- Starikova PK, Bykov RO, Itani TM, CHalapa VI, Sergeev AG, Olen'kova OM, i dr. V. Etiologicheskaya struktura enterovirusnogo meningita v Ekaterinburge do i posle pandemii COVID 19. Ural'skij medicinskij zhurnal. 2024; 23 (3): 26–35. Dostupno po ssylke: https://doi.org/10.52420/umj.23.3.26. Russian.
- Butakova LV, Sapega EYu, Trocenko OE. Enterovirusy — vozbuditeli gerpanginy u naseleniya Dal'nego Vostoka Rossii. Byulleten' fiziologii i patologii dyhaniya. 2025; (97): 57–68. Dostupno po ssylke: https://doi.org/10.36604/1998-5029-2025-97-57-68. Russian.
- Sapega EYu, Butakova LV, Trocenko OE. Osobennosti epidemicheskogo processa enterovirusnoj infekcii v Irkutskoj oblasti v 2023 godu. Zdorov'e naseleniya i sreda obitaniya — ZNiSO. 2024; 32 (8): 77–84. Dostupno po ssylke: https://doi.org/10.35627/2219-5238/2024-32-8-77-84. Russian.
- Nix WA, Oberste MS, Pallansch MA. Sensitive, seminested PCR amplification of VP1 sequences for direct identification of all enterovirus serotypes from original clinical specimens. J Clin Microbiol. 2006; 44 (8): 2698–704. DOI: 10.1128/JCM.00542-06.
- Kroneman A, Vennema H, Deforche K, Avoort H, Penaranda S, Oberste MS, et al. An automated genotyping tool for enteroviruses and noroviruses. J Clin Virol. 2011; 51 (2): 121–5. DOI: 10.1016/j.jcv.2011.03.006.
- Altschul SF, Gish W, Miller W, Myers EW, Lipman DJ. Basic local alignment search tool. J Mol Biol. 1990; 215 (3): 403–10. DOI: 10.1016/S0022-2836(05)80360-2.
- MedCalc Software Ltd. Fisher exact probability. Available from: https://www.medcalc.org/en/calc/fisher.php (Version 23.4.5; accessed December 12, 2025).
- Gaunt E, Harvala H, Österback R, Sreenu VB, Thomson E, Waris M, Simmonds P. Genetic characterization of human coxsackievirus A6 variants associated with atypical hand, foot and mouth disease: a potential role of recombination in emergence and pathogenicity. J Gen Virol. 2015; 96 (5): 1067–79. DOI: 10.1099/vir.0.000062.
- Puenpa J, Vongpunsawad S, Österback R, Waris M, Eriksson E, Albert J, et al. Molecular epidemiology and the evolution of human coxsackievirus A6. J Gen Virol. 2016; 97 (12): 3225–31. DOI: 10.1099/jgv.0.000619.
- Li X, Chen S, Chen Y, Han S, Dai B, Li T, et al. Epidemiological and genetic characterizations of hand, foot, and mouth disease and acute respiratory infections due to CV-A6 infection in Henan Province, China between 2021 and 2022. BMC Pediatr. 2025; 25 (1): 264. DOI: 10.1186/s12887-025-05527-6.
- Justino MCA, da S Mesquita D, Souza MF, Farias FP, Dos S Alves JC, Ferreira JL, et al. Atypical hand-foot-mouth disease in Belém, Amazon region, Northern Brazil, with detection of coxsackievirus A6. J Clin Virol. 2020; 126: 104307. DOI: 10.1016/j.jcv.2020.104307.
- Anh NT, Nhu LNT, Van HMT, Hong NTT, Thanh TT, Hang VTT, et al. Emerging coxsackievirus A6 causing hand, foot and mouth disease, Vietnam. Emerg Infect Dis. 2018; 24 (4): 654–62. DOI: 10.3201/eid2404.171298.
- Mirand A, Cohen R, Bisseux M, Tomba S, Sellem FC, Gelbert N, et al. A large-scale outbreak of hand, foot and mouth disease, France, as at 28 September 2021. Euro Surveill. 2021; 26 (43): 2100978. DOI: 10.2807/1560-7917.ES.2021.26.43.2100978.
- Hu L, Maimaiti H, Zhou L, Gao J, Lu Y. Changing serotypes of hand, foot and mouth disease in Shanghai, 2017–2019. Gut Pathog. 2022; 14 (1): 12. DOI: 10.1186/s13099-022-00485-1.
- Xu S, Li H, Qiao P, Xu G, Zhao D, Lin X, et al. Neonatal hand, foot, and mouth disease due to coxsackievirus A6 in Shanghai. BMC Pediatr. 2020; 20 (1): 364.
- Zhu P, Ji W, Li D, Li Z, Chen Y, Dai B, et al. Current status of hand-foot-and-mouth disease. J Biomed Sci. 2023; 30 (1): 15. DOI: 10.1186/s12929-023-00908-4.
- Chen L, Yao XJ, Yang H, Zhang HL, Shi XL, Peng B, et al. Molecular Epidemiology of Coxsackievirus A10 Associated With Hand, Foot and Mouth Disease From 2021 to 2024 in Shenzhen, China. J Med Virol. 2025; 97 (8): e70552. DOI: 10.1002/jmv.70552.
- Lv S, Zhou Y, Ji J, Yan Y, Zhu G. Epidemiological and genetic characteristics of enteroviruses associated with hand, foot, and mouth disease in Jiaxing, China from 2019 to 2022. Sci Rep. 2025; 15 (1): 14546. DOI: 10.1038/s41598-025-99251-x.
- Kokoreva SP, Kazarceva NV. Izmeneniya mochevoj sistemy u detej pri enterovirusnoj infekcii. Rossijskij pediatricheskij zhurnal. 2021; 24 (3): 193–6. Dostupno po ssylke: https://doi.org/10.46563/1560-9561-2021-24-3-193-196. Russian.
- Tapparel C, Siegrist F, Petty TJ, Kaiser L. Picornavirus and enterovirus diversity with associated human diseases. Infect Genet Evol. 2013; 14: 282–93. DOI: 10.1016/j.meegid.2012.10.016.
- Apostol LN, Suzuki A, Bautista A, Galang H, Paladin FJ, Fuji N, et al. Detection of non-polio enteroviruses from 17 years of virological surveillance of acute flaccid paralysis in the Philippines. J Med Virol. 2012; 84 (4): 624–31. DOI: 10.1002/jmv.23242.
- Holm-Hansen CC, Midgley SE, Fischer TK. Global emergence of enterovirus D68: a systematic review. Lancet Infect Dis. 2016; 16 (5): e64–75. DOI: 10.1016/S1473-3099(15)00543-5.
- Coramusi C, Rizzoli A, Alegiani C, Bonafoni S, Auriti C, Parisi P, et al. Neonatal Meningitis Due to Herpes Simplex Virus Type 1 and Enterovirus Coinfection: Case Report and Review of the Literature. Viruses. 2025; 17 (6): 790. DOI: 10.3390/v17060790.
- Nakata K, Kashiwagi M, Masuda M, Shigehara S, Oba C, Murata S, et al. A child with acute encephalopathy associated with quadruple viral infection. Front Pediatr. 2015; 3: 26. DOI: 10.3389/fped.2015.00026.
- Aguado I, Calvo C, Wilhelmi I, Pablo-Hernando ME, Medina MJ, Sáez-Nieto JA, et al. Sepsis and meningitis caused by Pasteurella multocida and echovirus 9 in a neonate. Pediatr Infect Dis J. 2014; 33 (12): 1308–9. DOI: 10.1097/INF.0000000000000504.
- Ndiaye N, Teixeira DD, Dia N, Da Silva Leite CC, Fall G, Furtado UD, et al. An outbreak of atypical hand, foot and mouth disease associated Coxsackievirus A6 in children from Cape Verde, 2023. Virol J. 2025; 22 (1): 48. DOI: 10.1186/s12985-025-02621-0.
- Hooi PS, Chua BH, Lee CS, Lam SK, Chua KB. Hand, foot and mouth disease: University Malaya Medical Centre experience. Med J Malaysia. 2002; 57 (1): 88–91. PMID: 14569726.
- Calvo C, Gallardo P, Torija P, et al. Enterovirus neurological disease and bacterial coinfection in very young infants with fever. J Clin Virol. 2016; 85: 37–39. DOI: 10.1016/j.jcv.2016.10.020.